Secure dental treatment with convenient, flexible financing solutions readily available and accessible.
Same Day Appointment Available, We Can Help You, Providing Quality Care For Your Emergency Dental Needs.
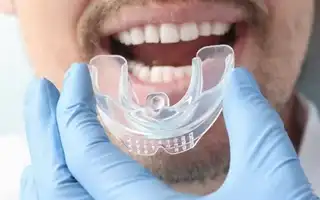
Passionate about ensuring the best care for sleep apnea patients’ restful sleep.
Select your preferred service and book a dentist visit in minutes. We’ll remind you of your appointment by SMS
YOUR DENTAL TEAM


CLIENT TESTIMONIALS
Get your hands on complimentary brochures and eBooks
Dental Services
WORKING HOURS
CONTACT DETAILS

At Korel Family Dentistry in San Diego, CA we believe a beautiful smile reflects your well-being and confidence. Our dedicated team provides tailored care for your needs, ensuring a healthy and dream smile. From routine to cosmetic treatments, our state-of-the-art facilities and compassionate approach guarantee outstanding results. Schedule your appointment today for a brighter smile!
Website Links
The information on this website is for general information purposes only. Nothing on this site should be taken as medical advice for any individual case or situation. This information is not intended to create, and receipt or viewing does not constitute, a doctor-patient relationship. Website Crafted with Love and Coffee by SandiWeb® : Web Development and Marketing Solutions. ©1998 – 2024. Korel Family Dentistry All Rights Reserved.